In summary:
- The Newborn Blood Spot (NBS) test is a crucial screening procedure performed around day 5 to check for 9 rare but serious inherited conditions.
- It is not a diagnostic test; an unusual result triggers further, more definitive testing to confirm a diagnosis and begin early treatment.
- Results can include being a “carrier” for a condition like cystic fibrosis, which has no health impact on your baby but is important genetic information for the wider family.
- While screening is strongly recommended by the NHS to prevent severe disability or death, parents have the right to decline the test for their baby.
For expectant parents in the UK, the “heel prick” test is a key milestone noted in the flurry of early appointments. Often mentioned as a routine check, the profound medical significance of this simple blood spot can be lost in the exhaustion of new parenthood. This isn’t just a tick-box exercise; it is a sophisticated piece of preventative medicine. The Newborn Blood Spot (NBS) screening programme is designed to detect nine rare but serious inherited conditions early, before a baby shows any signs of illness. Early detection and treatment are paramount, as they can significantly improve health outcomes and, in some cases, prevent severe disability or even death.
The conditions screened for include congenital hypothyroidism (CH), sickle cell disease (SCD), cystic fibrosis (CF), and six inherited metabolic diseases: phenylketonuria (PKU), medium-chain acyl-CoA dehydrogenase deficiency (MCADD), maple syrup urine disease (MSUD), isovaleric acidaemia (IVA), glutaric aciduria type 1 (GA1), and homocystinuria (HCU). Each of these conditions disrupts a specific biochemical pathway, and the screening test looks for the chemical markers that indicate such a disruption. While many parents focus on the brief discomfort of the procedure itself, the real questions often arise later: what happens if the test needs to be repeated? What does a “carrier” result mean? And how does this single test fit into the broader picture of our family’s genetic health?
This article moves beyond a simple list of conditions. It adopts the perspective of a clinical biochemist to explain the scientific and ethical logic behind the screening process. Instead of seeing the test as a single, pass/fail event, we will explore it as the first chapter in your child’s health story—a source of vital information that empowers parents to understand, to act, and to plan for a healthy future. We will examine how to manage the procedure, interpret the nuances of the results, and understand its connection to your wider family’s health history.
This guide provides a detailed look into the most common questions and concerns parents have about the Newborn Blood Spot test, from the practicalities of the procedure to the long-term implications of the results. The following sections are structured to give you clear, fact-based answers.
Summary: A Complete Overview of the Newborn Blood Spot Test
- How to Comfort Your Baby During the Heel Prick to Minimise Distress?
- What Does a ‘Carrier’ Result for Cystic Fibrosis Mean for Your Family?
- Why Do Repeat Tests Happen and Why Should You Stay Calm?
- When Should You Chase Your Health Visitor If NBS Results Are Delayed?
- Can You Opt Out of the Heel Prick Test and What Are the Legal Implications?
- Short Parents, Tall Child: Can Genetics Skip a Generation?
- Genetic Testing: Should You Test Your Child for BRCA if You Are Positive?
- Family Health History: When Should You Tell Your Doctor About Grandad’s Heart Attack?
How to Comfort Your Baby During the Heel Prick to Minimise Distress?
The heel prick procedure, while quick, inevitably causes some brief discomfort. A common concern for parents is how to minimise their baby’s distress. Fortunately, there are evidence-based techniques that can provide significant comfort. The primary goal is to activate the baby’s calming reflex. This can be achieved through a combination of holding, feeding, and swaddling. Holding your baby skin-to-skin is highly effective, as the warmth and familiar scent are naturally soothing. Breastfeeding during the procedure is also recommended, as the act of sucking and the sweetness of the milk have analgesic effects.
Beyond these immediate actions, a well-established technique known as the “5 S’s” can be incredibly effective for calming a fussy baby during and after any stressful event, including the heel prick test. This method, developed by paediatrician Dr. Harvey Karp, is designed to mimic the sensations of the womb. The five steps are Swaddling, Side or Stomach Position, Shushing, Swinging, and Sucking. Each step triggers a neurological response that helps to deactivate the baby’s crying and anxiety. These are not just folk remedies; they are based on a physiological understanding of a newborn’s reflexes.

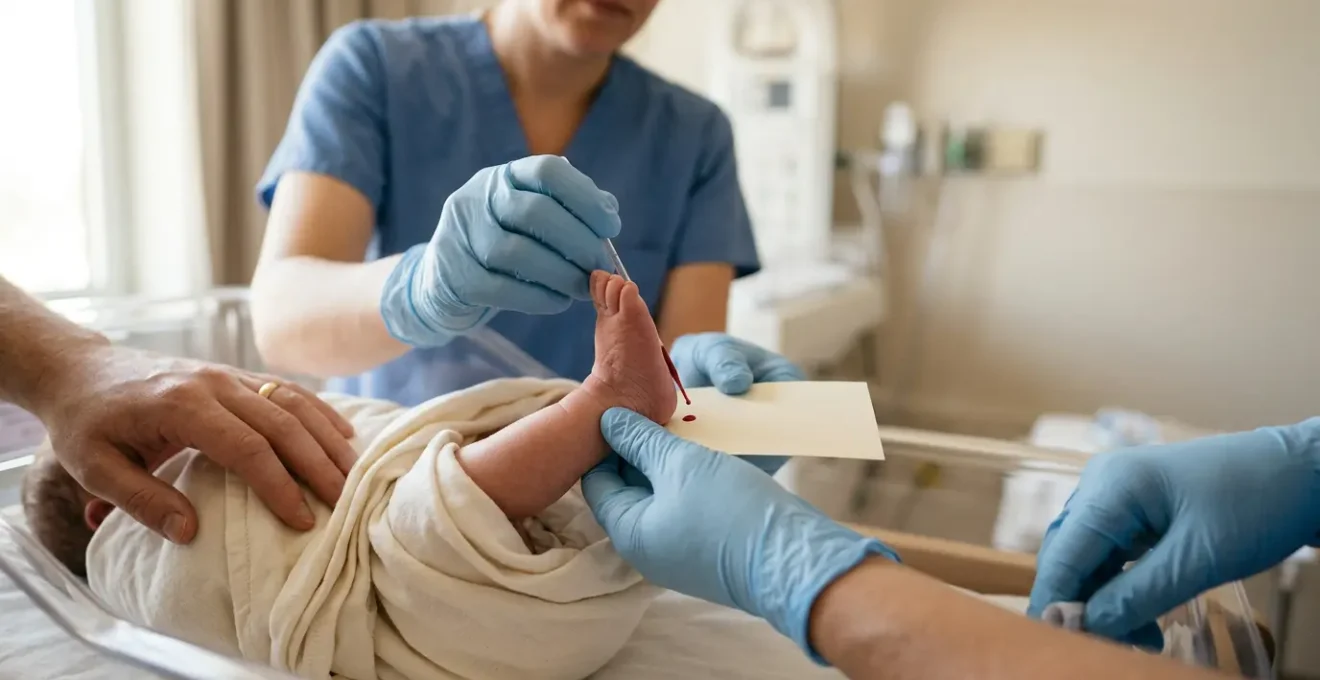
As the image illustrates, a snugly swaddled baby held in a secure position feels safe and contained, which prevents the Moro (startle) reflex that can escalate crying. The other components work in concert: a loud “shushing” sound replicates the constant noise inside the womb, gentle rhythmic motion soothes the vestibular system, and offering a pacifier or finger to suck on provides powerful, calming input. Mastering these techniques provides parents with a reliable toolkit for navigating not just the heel prick test, but many other challenging moments in the newborn period.
- Swaddling: Wrap your baby snugly in a blanket with arms at their sides to mimic the secure feeling of the womb and prevent the startle reflex.
- Side or Stomach Position: Hold your baby on their side or stomach over your shoulder while awake (always place on back for sleep) to activate their calming reflex.
- Shushing: Make a loud ‘shhh’ sound close to your baby’s ear, matching the volume of their cry, to replicate the womb’s noise level.
- Swinging: Use gentle, rhythmic motion by rocking or swaying your baby, with faster movement for upset babies and slower for calm ones.
- Sucking: Offer a pacifier, clean finger, or breast to trigger the natural sucking reflex, which lowers heart rate and stress levels.
What Does a ‘Carrier’ Result for Cystic Fibrosis Mean for Your Family?
Receiving a letter that mentions an “unusual” result from the newborn screening test is a source of significant anxiety for any parent. One of the most common follow-up findings is that the baby is a “carrier” for cystic fibrosis (CF). It is absolutely critical to understand what this means from a clinical perspective. A carrier result is not a diagnosis of cystic fibrosis. The baby is healthy and will not develop the disease. A carrier has one copy of the altered CF gene (the CFTR gene) and one working copy. To have cystic fibrosis, an individual must inherit two altered copies of the gene, one from each parent.
A CF carrier is healthy and does not have the disease.
– Cystic Fibrosis Foundation, Carrier Testing for Cystic Fibrosis Information Page
The clinical significance of a carrier result is not for the baby’s immediate health, but rather for the family’s future reproductive planning. If a baby is a CF carrier, it means that at least one of the parents must also be a carrier. If it is then discovered that the other parent is also a carrier, any future children that couple has will face a specific pattern of inheritance. For each pregnancy, there is a 25% chance the baby will have CF, a 50% chance the baby will be a carrier, and a 25% chance the baby will not have CF and will not be a carrier. This knowledge, discovered through the newborn screening test, is powerful information that allows family members (including aunts, uncles, and cousins) to make informed choices about their own carrier testing.
Therefore, a carrier result should be reframed from a source of fear into a piece of crucial genetic information. It provides an opportunity to understand the family’s genetic landscape better. Parents of a carrier baby will be offered an appointment with a genetic counsellor to discuss the implications, arrange testing for themselves if desired, and understand the options available for future pregnancies. This is a perfect example of how the NBS test provides proactive health information far beyond the immediate health of the newborn.
Why Do Repeat Tests Happen and Why Should You Stay Calm?
Being asked to return for a repeat blood spot test can be alarming, but it is a relatively common occurrence and, in the vast majority of cases, does not indicate a problem with your baby’s health. From a laboratory perspective, there are several clear, non-medical reasons why a repeat sample might be necessary. The most frequent cause is an insufficient sample. To perform all the required analyses, the lab needs a specific amount of blood to fully saturate the circles on the collection card. If the sample is too small, the tests simply cannot be run accurately.
Other technical reasons for a repeat test include issues with the collection process, such as a sample that was collected too early (before 5 full days of life), a sample damaged by heat or moisture during transport, or analytical issues in the lab. For example, a baby who is premature or has a low birth weight may have borderline results for certain markers that require a follow-up sample a few weeks later to see if they have normalised. Finally, there can be analytical interference, where something in the blood sample—like medication given to the baby or mother—interferes with the test, requiring a new, “cleaner” sample.

It’s important to remember that the screening programme is designed with a high degree of sensitivity to avoid missing any affected babies. This means the initial cut-off values for a “normal” result are very strict. A result that falls in a borderline or equivocal range will automatically trigger a request for a repeat test to be on the safe side. This is a feature of a robust quality control system, not a sign of imminent crisis. UK screening programmes have also become much more efficient; a study found that 81.4% of repeat samples were received by the lab within 10 days in 2020, a significant improvement from previous years.
The key is to follow the instructions provided by your midwife or health visitor promptly. The sooner the repeat sample is collected, the sooner you will have a definitive answer. While the wait is stressful, the statistical likelihood is overwhelmingly that the repeat test will come back as normal.
When Should You Chase Your Health Visitor If NBS Results Are Delayed?
After the heel prick test is performed, the waiting period for results can be a source of quiet anxiety. The official NHS guidance provides a clear timeline for parents. The vast majority of families—around 99 out of 100—will have a normal result and may not hear anything back at all. The principle is “no news is good news.” For those whose baby needs further testing, the NHS will contact them directly before the baby is 6 to 8 weeks old. Therefore, the standard expectation is that you should receive all necessary information within this period.
The NHS states that results are typically available within 6 weeks of the test being taken. This timeframe accounts for the sample’s transit to the regional screening laboratory, the complex analytical process, and the communication of results back to the local health trust. It is reasonable to wait until your baby is at least 6 weeks old before making any non-urgent enquiries. Chasing results too early can put unnecessary strain on healthcare services and will likely not yield any information, as the process may simply not be complete.
If you have not been contacted by the time your baby is 6 weeks old and you would like confirmation for your peace of mind, it is entirely appropriate to get in touch with your health visitor. When you call, it is helpful to approach the conversation calmly and with the necessary information at hand. Preparing your baby’s full name, date of birth, and NHS number will make the process much smoother for the healthcare professional looking up the records. Adopting a low-anxiety approach, framing it as a routine check-in, is often the most effective way to get the reassurance you need without causing undue alarm.
Your Action Plan: Following Up on Delayed Results
- Wait for the Standard Timeline: Do not make a non-urgent enquiry before your baby is at least 6 weeks old, as this is the normal processing window.
- Prepare Your Baby’s Details: Before calling, have your baby’s full name, date of birth, and the date of the test ready.
- Use a Calm and Clear Script: Politely state you’re calling for a routine check on the blood spot results as you haven’t heard anything and would like confirmation.
- Follow Up Proactively for Repeats: If a repeat test was performed, follow up within the specific timeline given by your healthcare provider rather than waiting the full 6 weeks.
- Know Who to Contact: Your primary point of contact is your health visitor, but your midwife or GP surgery can also access the screening records.
Can You Opt Out of the Heel Prick Test and What Are the Legal Implications?
The principle of informed consent is central to all medical procedures in the UK, including newborn screening. While the NHS strongly recommends the blood spot test for all babies due to its proven ability to save lives and prevent serious disability, it is not mandatory. Parents have the legal right to decline the screening for their child. This choice, however, should be made only after a full and clear discussion with a healthcare professional about the potential consequences.
The clinical implications of opting out are significant. Declining the test means that the nine serious conditions will not be screened for. If a baby has one of these conditions, it will likely not be detected until they become visibly unwell. By that time, irreversible harm, such as brain damage from untreated PKU or a life-threatening crisis from MCADD, may have already occurred. The entire purpose of the NBS programme is to intervene before symptoms appear. This is why the medical community’s recommendation is universal and unequivocal.
The overwhelming parental consensus supports this view. For instance, data from neighbouring countries shows similar trends; 99.9% of parents in Ireland agree to have their babies screened, highlighting the near-universal acceptance of the test’s benefits. The decision to decline is rare but respected. If parents choose to opt out, they will be asked to sign a form confirming their decision and that they have understood the risks involved. This is documented in the baby’s health records.
The NHS recommends NBS screening because it can improve health and prevent severe disability or even death. However, screening is always a choice and parents can decline it for their baby if they wish.
– NHS England, Newborn Blood Spot Screening Programme Overview
Ultimately, the legal position is clear: you can opt out. The ethical and medical position is equally clear: the benefits of screening are so profound that opting in is one of the most important early decisions a parent can make for their child’s long-term health. The test empowers parents with knowledge and protects the child from preventable harm.
Short Parents, Tall Child: Can Genetics Skip a Generation?
The question of how traits like height are inherited is a common source of family discussion. It is entirely possible for parents of average or short stature to have a tall child, and this doesn’t necessarily mean a gene has “skipped a generation” in the way one might think. Height is a polygenic trait, meaning it is influenced by hundreds, if not thousands, of different genes, each contributing a small effect. A child inherits a unique combination of these genes from both parents, and this specific mix can result in a height that is significantly different from either parent.
Furthermore, environmental factors play a crucial role. Optimal nutrition, healthcare, and overall well-being during childhood and adolescence can help a child reach their maximum genetic height potential, which may be greater than that achieved by previous generations who may have had different environmental conditions. The concept of traits “skipping a generation” is more accurately applied to single-gene recessive conditions, where a person can be a healthy carrier of a trait and pass it on to a child who may then express the trait if their other parent is also a carrier.
This is where the Newborn Blood Spot test provides a critical distinction. While complex traits like height are not screened for, the test is specifically designed to detect serious single-gene or metabolic conditions that can severely impact growth and development. A key example is Congenital Hypothyroidism (CH), one of the nine conditions on the UK screening panel.
Congenital hypothyroidism is a rare condition which can lead to impaired growth and mental development.
– Patient.info, Newborn Blood Spot Test (Screening) Information
Without the early detection and treatment made possible by the NBS test, a baby with CH would fail to produce enough thyroid hormone, leading to stunted growth and permanent intellectual disability. A child’s failure to grow as expected is a significant medical red flag. The screening test ensures that a treatable hormonal cause like CH is identified and managed from the first weeks of life, allowing the child to grow and develop normally. This highlights the difference between normal genetic variation in height and a pathological failure to grow, which the NBS test is designed to prevent.
Genetic Testing: Should You Test Your Child for BRCA if You Are Positive?
If a parent knows they carry a genetic mutation like BRCA1 or BRCA2, which significantly increases the risk of adult-onset cancers, it is natural to question whether their children should be tested. However, the medical and ethical consensus is firm: predictive genetic testing for adult-onset conditions is not recommended for minors. This stance can seem counterintuitive when compared to the universal recommendation for newborn screening. The key difference lies in the principle of clinical actionability in childhood.
The Newborn Blood Spot test screens for conditions where immediate treatment or intervention during infancy can prevent irreversible harm. For a baby with PKU, starting a special diet in the first days of life prevents severe brain damage. For a baby with CH, daily thyroid hormone medication allows for normal growth and brain development. In every case on the NBS panel, there is a clear, established, and effective medical intervention that must begin in childhood.
This is not the case for adult-onset conditions like those associated with BRCA mutations. There is no treatment or preventative measure that would be taken during childhood. The increased cancer risk does not manifest until adulthood, typically after the age of 30. Testing a child provides no immediate health benefit and instead removes their future autonomy—their right to decide for themselves, as an adult, whether they want to know this information. Professional genetics societies worldwide advise against this, preserving the child’s “right not to know.” The following table clarifies the fundamental ethical differences between these two types of testing.
| Principle | NBS (Newborn Blood Spot Screening) | Predictive Testing (e.g., BRCA in Children) |
|---|---|---|
| Actionability in Childhood | Immediate treatment available for all screened conditions (e.g., PKU diet, thyroid medication) | No treatment or intervention available until adulthood |
| Age of Disease Onset | Conditions manifest in infancy or early childhood without intervention | Increased cancer risk manifests in adulthood (typically 30+ years) |
| Child’s Future Autonomy | Screening enables the child to live a healthy childhood and make informed choices as an adult | Testing removes the child’s right to decide whether to know their genetic risk when they are mature enough to consent |
| Medical Consensus | Universally recommended by medical organizations globally | Not recommended by genetics professional societies for minors |
| Wilson-Jungner Criteria Alignment | Meets all criteria: important health problem, accepted treatment, reliable test, early detection beneficial | Fails criteria: no childhood intervention, no immediate benefit, compromises autonomy |
This framework, based on the internationally recognised Wilson-Jungner criteria for screening, demonstrates why NBS is a public health imperative, while predictive testing of children for adult-onset conditions is an ethical breach of their future autonomy.
Key Takeaways
- The Newborn Blood Spot (NBS) test is not a diagnostic tool but a highly sensitive screening test to identify babies who need further investigation.
- A “carrier” result is not a diagnosis; it means your baby is healthy but carries genetic information that may be relevant for future family planning.
- Repeat tests are common and often due to sample quality issues, not a health problem. The system is designed to be cautious to avoid missing any cases.
Family Health History: When Should You Tell Your Doctor About Grandad’s Heart Attack?
Discussing family health history with your doctor is a cornerstone of personalised and preventative medicine. Events like a grandparent’s heart attack are significant pieces of information, especially if they occurred at an early age (typically before 55-60), as this can indicate a hereditary predisposition to cardiovascular disease. However, the scope of relevant family history is often broader than many people realise. It is not just about major diseases; it also includes information revealed through genetic screening.
This is where the Newborn Blood Spot test plays an unexpected but crucial role. The screening process can uncover new genetic information in a family with no known history of a particular condition. For example, the UK government guidance highlights that newborn screening identifies some babies who are genetic carriers of conditions like cystic fibrosis or sickle cell disease, even when no one in the family was aware of the gene being present. This single test result effectively rewrites the family’s health history.
When a baby is identified as a carrier, it automatically provides clinically significant information about the parents and, by extension, the grandparents, aunts, uncles, and cousins. This new knowledge creates a responsibility to share this information, as it empowers relatives to seek testing and make informed decisions about their own health and reproductive choices. Discussing this with family can be delicate, but it is a profoundly helpful act. The conversation is not just about a single baby’s test result; it is about providing the entire family with a more complete and accurate picture of its shared genetic landscape.
Action Plan: How to Discuss a Carrier Result with Your Family
- Understand and Prepare: First, ensure you fully comprehend what being a carrier means—that it is not an illness—and plan to speak with immediate family (your parents and your partner’s) first.
- Craft a Clear Message: Use simple, non-alarming language. Explain that being a carrier means having one copy of a gene change, which is not harmful but can be passed to future children.
- Emphasize Generational Relevance: Share that this information could be important for siblings, cousins, and other relatives when they plan their own families, giving them the option for testing.
- Provide Official Resources: Offer to share information leaflets from your healthcare provider or suggest they speak with their GP or a genetic counsellor to get expert advice.
- Focus on Empowerment: Frame the conversation positively, as giving family members valuable knowledge that allows them to make informed choices for their future.
Therefore, your family health history is a living document. It should be updated not only with major events like a heart attack but also with new genetic information revealed through tests like the NBS. Sharing this complete picture with your doctor allows for the best possible care for you and your child.
Understanding the Newborn Blood Spot test is the first step in a lifetime of proactive health management for your child. For a more detailed breakdown of the conditions screened and the support available, discussing any concerns with your health visitor is always the best course of action.